For Administrators
Safe, Cost-Effective CRNA Care: Good for Hospitals, Good for Patients
In today’s rapidly changing healthcare environment, there is one constant that healthcare facility administrators can count on: the safe, cost-effective anesthesia care provided by Certified Registered Nurse Anesthetists (CRNAs).
CRNAs are highly qualified anesthesia experts who practice in most of the hospitals and ambulatory surgery centers across North Carolina where anesthesia is required for surgery, labor and delivery, trauma care, and pain management. In rural and other medically underserved counties of North Carolina, CRNAs are often the sole anesthesia professionals serving their communities.
CRNAs ensure that patients have access to essential anesthesia services and help facilities deliver exceptional anesthesia and related care efficiently and cost-effectively.
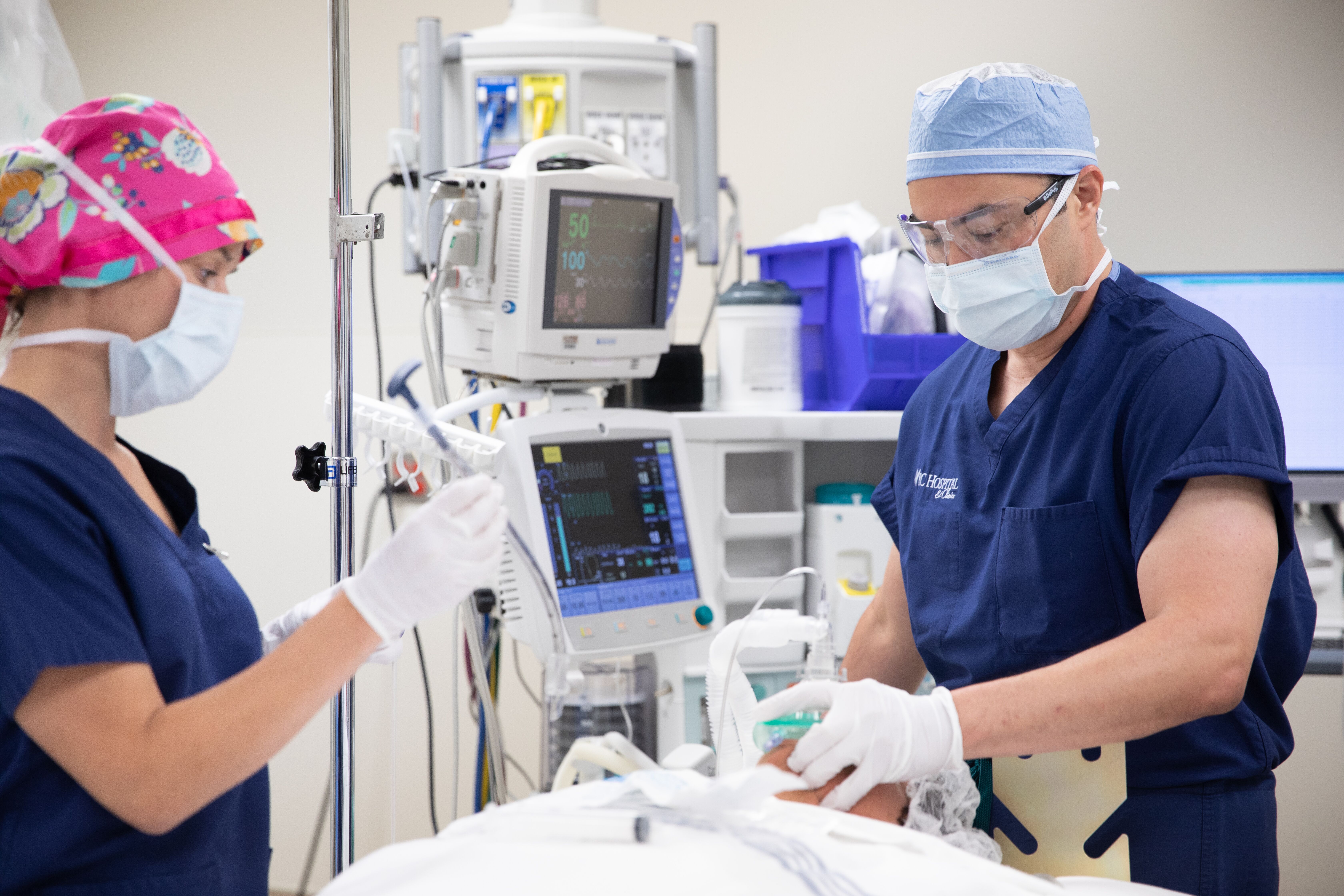
Meet NC’s CRNA Workforce
If a healthcare facility in North Carolina provides surgical, labor and delivery, emergency, pain management, or any other services that require anesthesia, it’s a safe bet that CRNAs are present to provide the anesthesia—every breath, every beat, every second. CRNAs are known for providing safe, compassionate hands-on patient care, and staying with their patients throughout their procedure. They are a respected member of the patient care team, working closely with other members of the team including surgeons or other types of physicians, nurses, and technicians. In facilities where CRNAs work with physician anesthesiologists, CRNAs typically are the hands-on providers of the anesthesia care delivered to patients.
- There are more than 3,400 licensed CRNAs in North Carolina.
- CRNAs provide anesthesia in all of North Carolina’s counties that have anesthesia services; there are no anesthesiologist-only counties.
CRNA education, training, and practice are extensive. Enabling these anesthesia experts to provide patient care to the full extent of their education, training, licensure and certification is in the best interests of healthcare facilities and the communities they serve. In short, CRNAs…
- Practice in collaboration with other qualified healthcare professionals.
- Provide safe, holistic, patient-centered, evidence-based anesthesia and analgesia services.
- Conduct a pre-anesthesia interview with the patient, administer the anesthetic, monitor and interpret the patient’s vital signs, manage the patient throughout surgery, and ensure the patient’s safe transfer to recovery.
- Are well prepared to handle any emergency.
- Provide anesthesia care in every healthcare setting where anesthesia is required for surgical, obstetrical, trauma, diagnostic, therapeutic, and pain management services.
- Care for patients of all ages and at every acuity level.
- Are the primary anesthesia providers for maternity patients, in rural and other medically underserved areas of the United States, and in the U.S. Military.
For a concise summary of the primary elements of nurse anesthesia practice, click here.
Research Confirms CRNA Safety and Cost-Effectiveness
According to the National Academy of Medicine, anesthesia is one of the safest healthcare experiences a patient can undergo. All significant anesthesia-related research published since 2000 has confirmed the safety of anesthesia care delivered by CRNAs, including the following landmark studies:
Based on the research, patients who undergo surgical and other procedures in hospitals and ambulatory surgery centers in CRNA-only counties can rest assured that they will receive the safest, most cost-effective anesthesia care available.
Risk Management
- Nationwide, the average 2018 malpractice liability insurance premium for self-employed CRNAs was 33 percent less than it was in 1988, and 68 percent less when trended for inflation—evidence that CRNA care today is safer than ever.
- Case law has repeatedly demonstrated that surgeons are no more liable when working with a CRNA than with an anesthesiologist.
How do CRNAs and Anesthesiologists Differ?
It is far more accurate to ask, “How are they similar?” CRNAs and anesthesiologists provide anesthesia care using the same techniques and medications, to patients of all ages, in every type of healthcare setting, for every type of procedure that requires anesthesia.
Nurse anesthetists were the first recognized anesthesia professionals in the United States and have been providing patients freedom from pain for more than 150 years.
There is one significant difference, however: Anesthesiologist compensation is approximately 2.5 times greater than that of CRNAs. Medicare pays the same fee for anesthesia services regardless of whether they are provided by a CRNA working solo, an anesthesiologist working solo, or a CRNA and anesthesiologist working together. Therefore, the anesthesiologist’s higher compensation is typically covered by the hospital, healthcare facility or the patient.
Need to Know Information
CRNAs Advocate for and Specialize in Enhanced Recovery After Surgery (ERAS®)
As healthcare professionals, policymakers, and other stakeholders continue to seek effective ways to combat the opioid crisis, CRNAs are doing their share to win the fight.
ERAS is a collaborative approach to pain management which involves the patient, CRNA, and entire care team. This patient-centered strategy relies on robust patient communication and opioid-sparing techniques such as regional anesthesia, peripheral nerve blocks, and non-opioid medications. ERAS reduces the need for opioids, improves patient outcomes, and reduces healthcare costs.
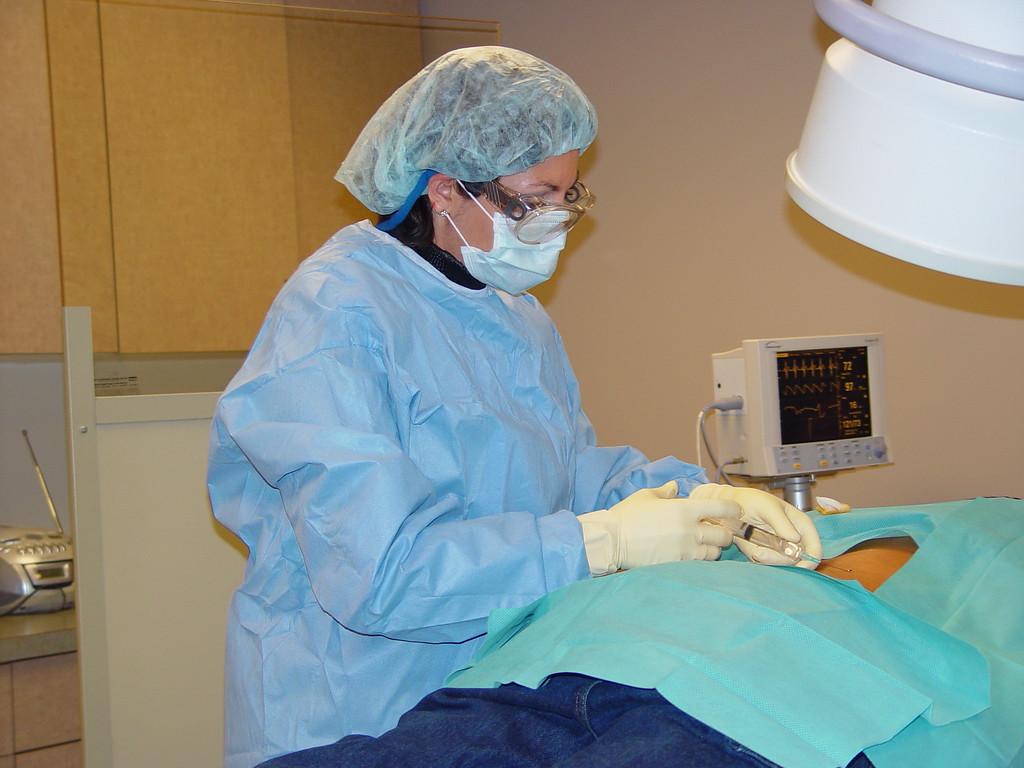
CRNAs are Pain Management Specialists
Chronic pain afflicts millions of Americans. CRNAs are specifically educated and trained to care for pain patients by delivering anesthetic injections around nerves and other treatments.
CRNAs were the First Nursing Specialty to be Granted Direct Reimbursement Rights under Medicare
Legislation passed by Congress made it official in 1986.
CRNA Education and Training
Total education and training:
- 7-8 ½ years of nursing and anesthesia education and training
- More than 9,000 clinical hours
Prior to entering nurse anesthesia program:
- Attain bachelor’s degree in nursing, RN license, minimum 1 year of critical care experience
- Average critical care experience: 2.9 years (CRNAs are the only anesthesia professionals who start their anesthesia education knowing how to manage critical events)
Prior to becoming a CRNA:
- Graduate with master’s or doctorate degree from accredited nurse anesthesia educational program
- Pass National Certification Exam
CRNAs embrace life-long learning, maintaining their certification through continuing education.
Learn More about CRNAs
Highly Educated Professionals Providing Safe, Affordable, Accessible Care
|



